At a time when health care systems around the globe are struggling to keep up with the influx of patients from the COVID-19 crisis, BD employees with clinical backgrounds are stepping up to help. Through their selfless acts, they show us what it means to live the BD purpose of advancing the world of health everyday and remind us why we’re #ProudToBeBD.
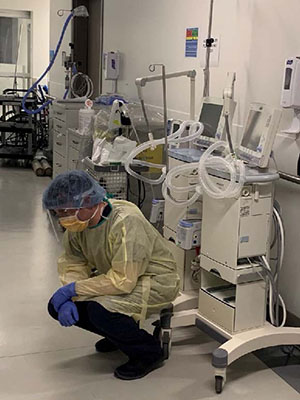
One of these amazing individuals, Adam Wires, RN, CVAA(C), VA-BC and a clinical specialist with BD – Canada, recently volunteered to serve alongside other healthcare heroes at a hospital in his local community.
Below is his personal account of the experience, which provides an eye-opening look into what clinicians and caregivers are facing as they address this crisis. It's also an important reminder of how critical it is to play our part in reducing the spread of the virus and continue to support health care workers through this difficult time.
I received a phone call from the program director at my local hospital asking if I could come in to assist within the Emergency Room (ER) over the weekend. Multiple staff had been sent home to self-isolate due to positive exposures over the past week; other staff had called in mentally fatigued and unwell, and Friday afternoon the ER saw a record breaking number of individuals with signs and symptoms of COVID-19.
After parking my car, I walked into what appeared to be a war zone. A long line of patients standing six feet apart lined up out the ER entrance door. People waiting to be seen by an ER physician, hoping to get screened and assessed for whatever ailment or symptom they might have. People walking in looking for masks, multiple people stealing isolation gowns, gloves and even standing in front of the automatic Purell dispensers filling up Tupperware containers of hand sanitizer.
The day staff were exhausted and, after receiving report, I quickly learned what the health care system is expecting to face over the next weeks (or months) to come. Three of my patients that night had to be intubated for acute respiratory distress most likely caused by COVID-19. One, a young secretary from a Family Health Practice, had a respiratory rate of 48 breaths per minute, and oxygen levels in the low 80's even though she was receiving full oxygen.
Constantly it was a repetitive task: mask on, gown on, hand washing, gown off, mask off… all night. Our hands dry and stinging from the frequent use of harsh hand sanitizer, soap or the rough paper towels. A simple task that would normally take just a few minutes now was a much longer ordeal. The need to have laboratory specimens double bagged and walked to the lab for analysis. “Clean” staff to get supplies from storerooms; the careful navigation of transferring suspected patients to other areas of the hospital; the constant phone calls from family checking on their loved ones (since no visitors are allowed). Just when you would get a patient out of the room, a new one was already lined up for that bed.
And bed space is in high demand. Vulnerable populations (i.e. those from the shelter system / homeless) cannot go back to their shelter, so the city has a designated hotel for these patients to self-isolate. That hotel was completely full just four days after opening. This resulted in us having to put three to four of them into a single room – sleeping in a reclining chair, no privacy, bagged meals and the constant noise of a busy emergency room.
Staff are afraid. Afraid that this pandemic isn’t going to go the way everyone thinks it will. While people complain about being stuck at home, these healthcare workers are putting themselves into the line of danger to care for those people who didn’t adhere to the warnings by our government. Worried that they will bring this virus home – sleeping in the basement, or even their cars to keep their loved ones safe.
Last night, one of my patients died from COVID-19. He had a long, complex history of respiratory problems - but this virus is running rampant in the homeless population. Standing by his side as his oxygen levels kept dropping. Listening to the thick gurgling secretions blocking his airway. I couldn’t let him die alone, standing for 40 minutes by his side, dressed in layers of protective equipment, holding his hand and reassuring him he wasn’t alone. It’s been a while since I had to deal with a patient dying, but no time to mourn, other sick patients waited.
This morning we ran out of isolation gowns. We were low on face shields. Reading the news about Washington State where the healthcare staff have reported no more PPE (personal protective equipment) left and had resorted to using ski goggles and bandanas for protection. And this is just the beginning.
Staff are being re-deployed throughout the hospital. Units are being converted to COVID-19 spaces. Policies and procedures change on a minute-by-minute, hour-by-hour basis. Staff leave fatigued, overwhelmed and exhausted – only to sleep for a few hours and return to it all over again.
Please remember to wash your hands. Avoid going out into public, only when essential. Listen to our health professionals and government. Together, we have the chance to decrease the severity of this pandemic. Together, we are strong.
Subscribe to receive BD blog alerts